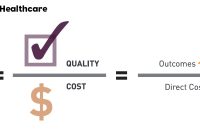
The Value Equation in Value Based Care
I have referenced, over the years, one way to measure value for those we serve. As we continue our journey, being able to quantify what we do is critical to our success. Attached is a link to an article published by the Advisory Board that goes into greater detail on the equation I have discussed. How Sentara measures… Read More »